1
Consultation and sperm donor search
An initial consultation is the first step to find out about the sperm donation procedure including donor selection process and costs. Our coordinators will work with you to assist in finding the right donor for you.
We work with accredited international sperm banks, and we ensure the selection of high-quality sperm from sperm donors of all races and ethnicities.
2
Recipient screening and Ovarian preparation
Your doctor will recommend some tests to ensure you are ready for treatment. These typically include a hormonal profile test, ovarian reserve test and an ultrasound scan. Your doctor will advise you to undergo a course of medication and monitoring which will help ensure the best possible results. During this period, you will have scans and blood tests to ensure the best outcome.
3
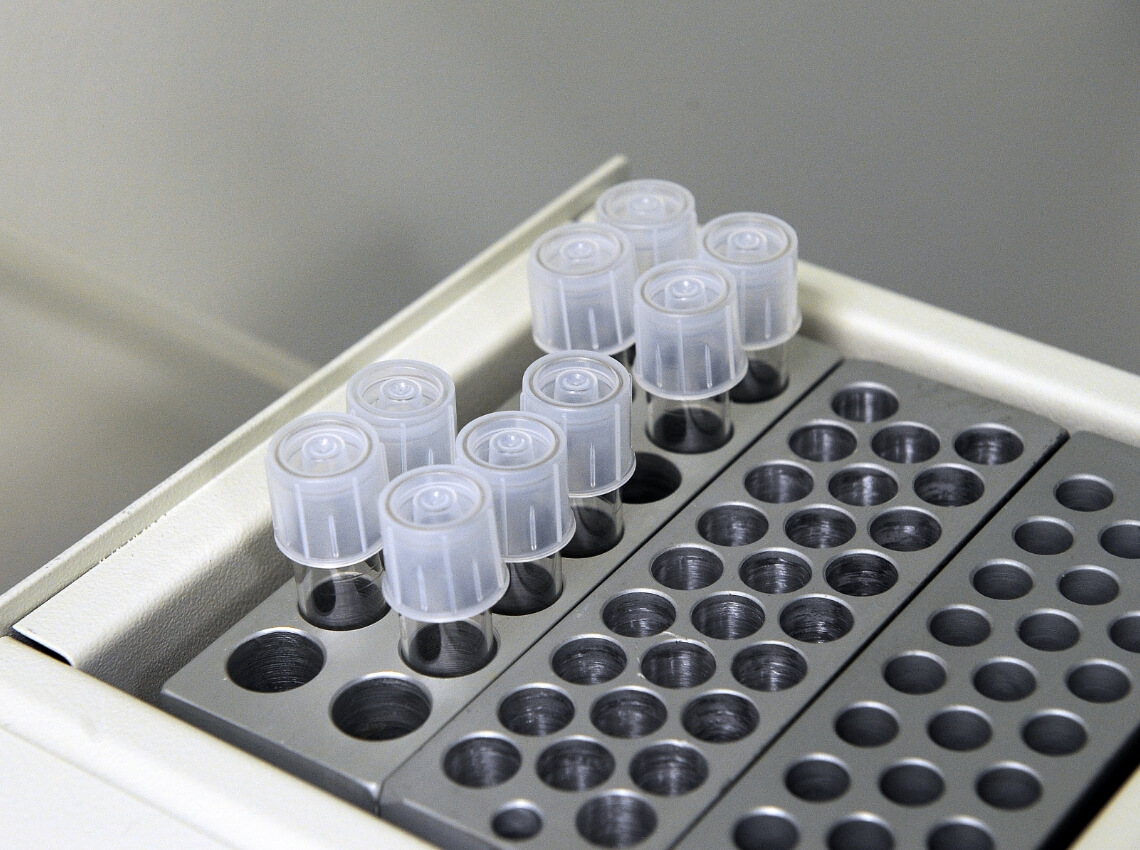
Egg collection
Having monitored your blood and scan result, your doctor will decide when the optimal time is to collect your eggs. The procedure involves collecting eggs from the woman’s ovaries using a needle that is passed through the vagina and into each ovary under ultrasound guidance and deep sedation.
4
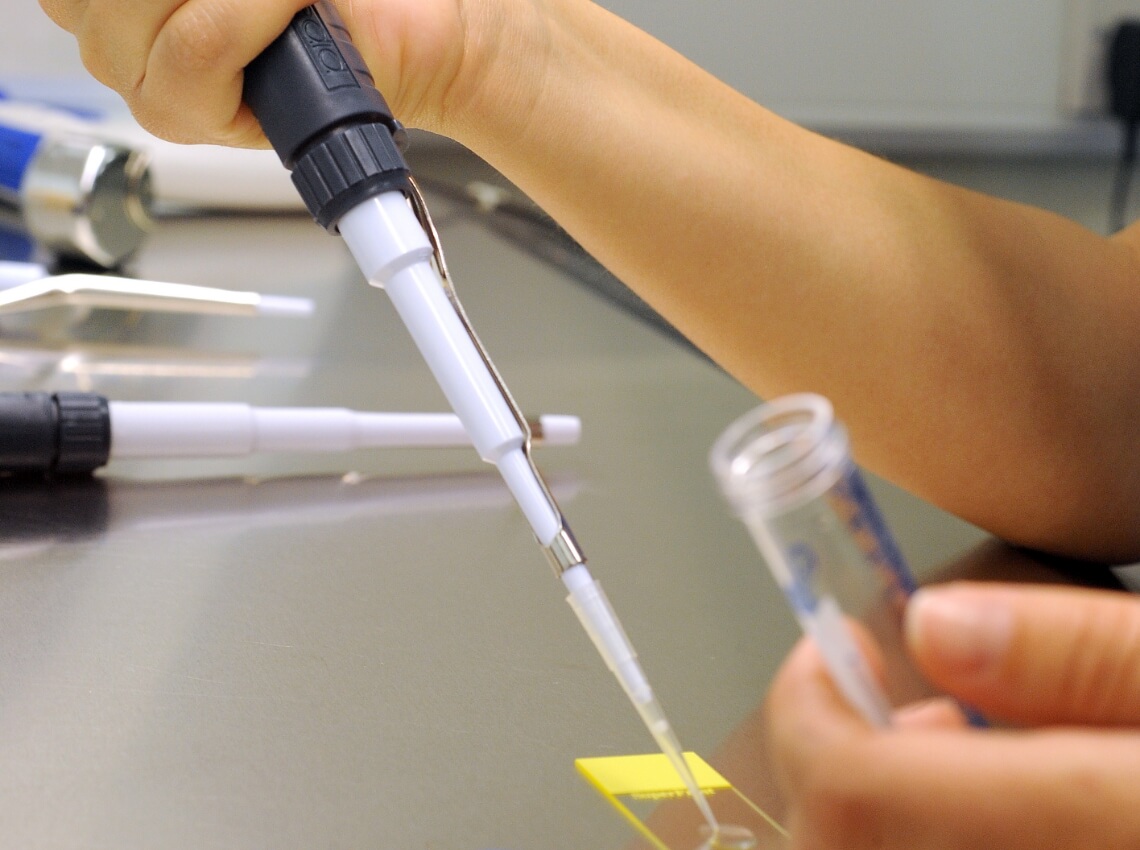
Fertilization and embryo development
On the day of the egg collection, the eggs will be fertilised with donor sperm in the laboratory. Embryos typically develop for 5 or 6 days prior to transfer or freezing. Our embryologists are in constant contact with you during this time to update you on your embryo's development.
5
Embryo transfer
Your doctor and embryologist will advise on medications that you should take to prepare the endometrium for the embryo transfer.
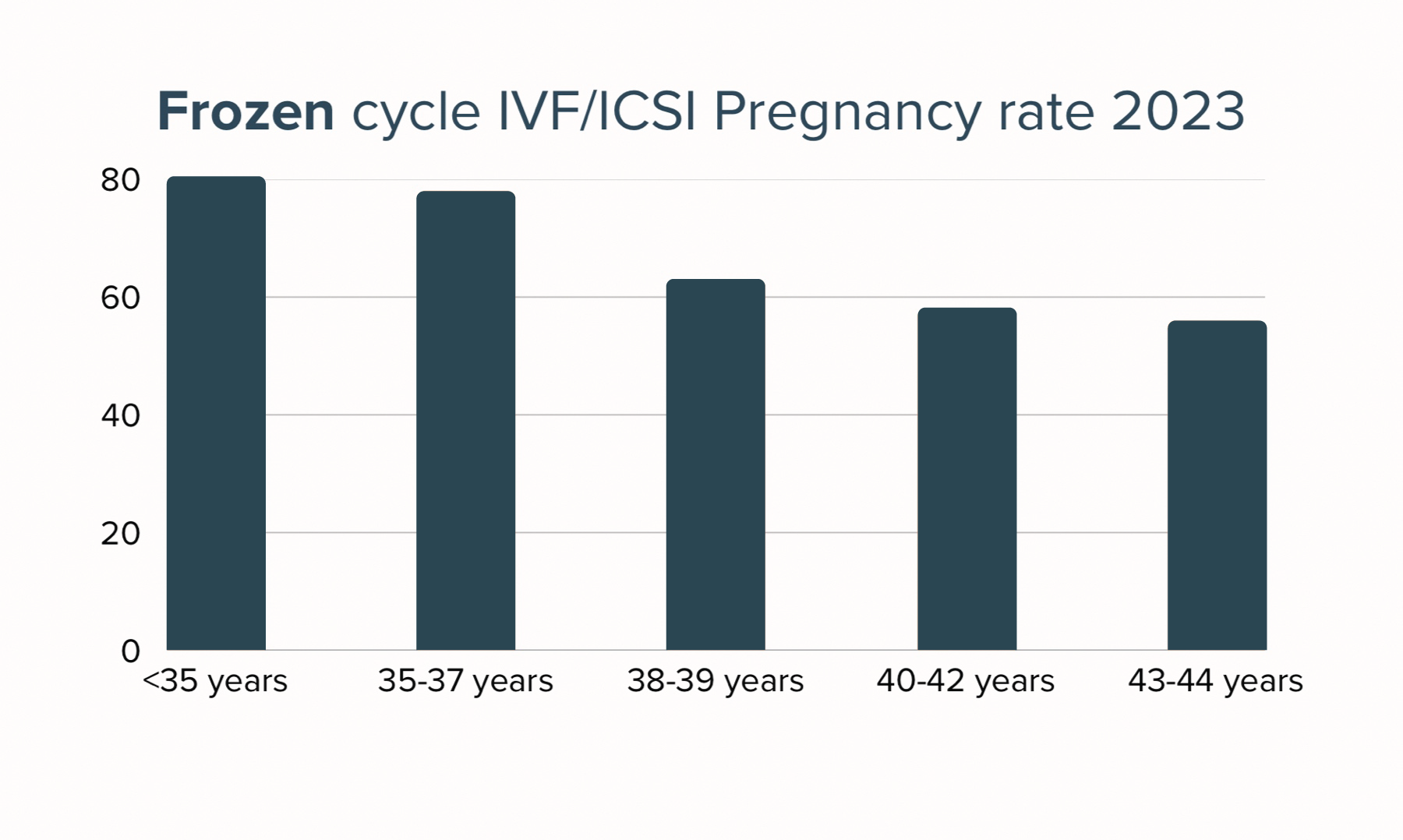
There are two ways to transfer an embryo: fresh or frozen embryo transfer. Either the embryo can be transferred back to the uterus five days after the fertilization, or the embryo(s) can be frozen and thawed for a transfer at a later stage. The embryologist will help you to decide which embryo is the best to transfer for the highest possible chance of a healthy and successful pregnancy.
6
Pregnancy test
9 days after your embryo transfer you will take a pregnancy test which will confirm the results of your treatment. Whatever the outcome, our team of doctors, embryologists, nurses and counsellors will be on hand to support you in your next steps.